Is It Really Trauma Bonding?
You see it everywhere now — social media posts, podcast discussions, conversations with friends. Someone had a difficult breakup, and suddenly: "I was trauma bonded." A coworker stays in an unfulfilling job: "Must be trauma bonding." A friend tolerates rude behavior from family: "That's trauma bonding, right?" The term has become cultural shorthand for "I stayed when I should have left." And while the widespread recognition represents real progress, something valuable — and potentially life-saving — gets lost when a clinical term becomes a catch-all for every painful relationship.
What Is a Trauma Bond?
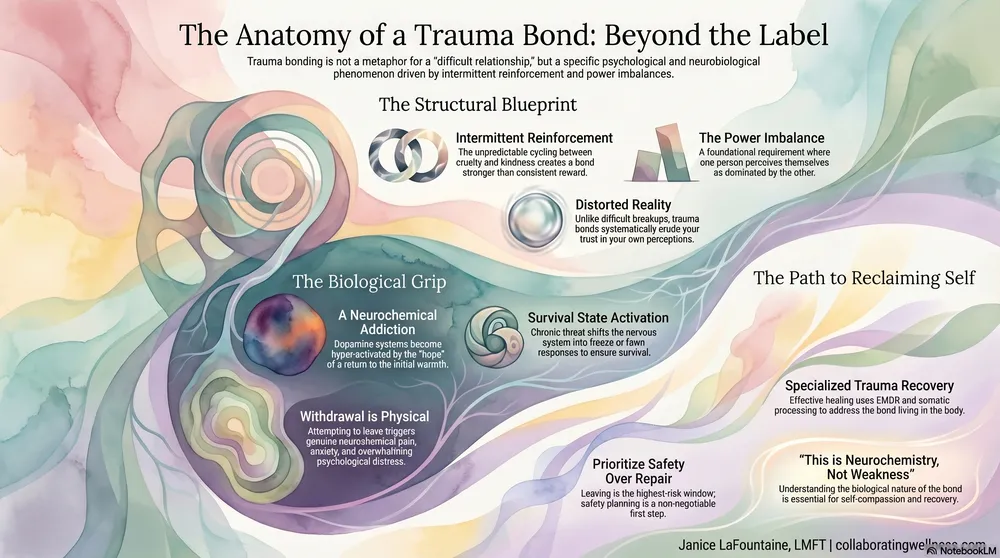
A trauma bond is an intense emotional attachment that forms between a person and someone who intermittently abuses them, created by the cycling of punishment and reward within a relationship marked by a significant power imbalance. The concept was first described by psychologists Donald Dutton and Susan Painter in 1981 and later expanded by Patrick Carnes in his 1997 book The Betrayal Bond. Trauma bonding is not a character flaw or a sign of weakness. It is a predictable neurobiological response to specific conditions — intermittent reinforcement and power differential — that hijack the brain's attachment and reward systems. The bond strengthens precisely because the abuse is unpredictable, not in spite of it. Understanding this distinction is critical because the term describes a specific pattern of psychological captivity that requires safety-focused intervention, not just better communication or stronger boundaries.
This article will help you distinguish between a genuine trauma bond and other painful relationship patterns that deserve attention but require different responses. That precision matters — because the right label points you toward the right help, and in some cases, the right label is what keeps you safe.
What Does "Trauma Bonding" Actually Mean in Clinical Terms?
Trauma bonding is a specific psychological phenomenon — not a metaphor for "hard to leave." Dutton and Painter's foundational research identified two structural features that must both be present: a power imbalance, where one person perceives themselves as dominated by the other, and intermittent abuse, where cruelty and kindness alternate unpredictably. Their 1993 empirical study of 75 women who had left abusive relationships confirmed that the severity of intermittent maltreatment and the degree of power differential predicted the strength of emotional attachment — not just at separation, but six months later.
Patrick Carnes expanded this framework in The Betrayal Bond, describing trauma bonds as "highly addictive attachment to the persons who have hurt the client most." Carnes identified that the bond forms through exploitation of trust and power, and that the resulting attachment functions like an addiction — complete with tolerance, withdrawal, and compulsive return. This isn't a relationship that's "hard to leave." It's a relationship that has restructured how the brain processes danger, reward, and attachment.
How Is a Trauma Bond Different From Just Staying in a Hard Relationship?
This is the question the reader usually comes here with, and the answer matters enormously. Many painful relationships are hard to leave. Grief, love, financial entanglement, children, shared history, fear of being alone — these are real forces that keep people in relationships that aren't working. None of them, by themselves, indicate a trauma bond.
The diagnostic fork is this: In a difficult but non-abusive relationship, you may feel sad, conflicted, or stuck — but you retain your sense of reality. You know what happened. You trust your own perceptions. In a trauma-bonded relationship, your reality has been systematically distorted. You question your own memory. You minimize clear abuse. You feel genuinely unable to leave even when you can articulate why you should — and the intensity of the connection feels like proof the relationship is special rather than proof it is dangerous.
If you recognize the second pattern, what you're dealing with isn't just emotional difficulty. It's coercive control — and it requires a specific kind of help.
In my work with clients in trauma-bonded relationships, the recognition moment often arrives not when a client realizes their partner is hurting them — they usually know that, somewhere — but when they notice how much labor they've been doing to keep the relationship looking better than it actually is. The minimizing, the softening, the rewriting in real time. When a client first describes an interaction without smoothing it, the room changes. The body knows. The bond starts loosening from the inside.
Why Does My Brain Feel Addicted to Someone Who Hurts Me?
Because, neurobiologically, it is. When you're in a trauma-bonded relationship, your brain's dopamine system — the seeking-and-wanting circuitry — becomes hyperactivated by the intermittent reward pattern. You're not addicted to the abuse. You're addicted to the hope of the reward: the return of that initial warmth, the next "good phase," the person you fell in love with before the mask slipped. Research on intermittent reinforcement schedules shows this pattern creates the strongest, most extinction-resistant behavioral bonds — stronger than consistent reward, stronger than consistent punishment.
Meanwhile, your bonding system — driven by oxytocin and endogenous opioids — ensures that any attempt to leave triggers genuine neurochemical withdrawal: grief, anxiety, panic, and overwhelming psychological pain. As Bessel van der Kolk's research in The Body Keeps the Score documents, chronic relational trauma literally alters how the brain processes threat and safety. The constant stress of the abusive environment doesn't weaken the bond — it amplifies it. The highs feel more euphoric because the baseline is so painful. The withdrawal feels unbearable because your nervous system has recalibrated around the relationship as its primary source of regulation.
Stephen Porges' polyvagal theory adds another layer: under conditions of chronic threat, the nervous system shifts into survival states — freeze, fawn, appease — that look from the outside like "choosing to stay." They aren't choices. They're the body's best available strategy for surviving a situation it has correctly identified as dangerous. This is neurochemistry, not weakness.
What Are the Stages of a Trauma Bond?
Drawing on Carnes and later trauma-bonding literature, a recognizable progression emerges. Not every trauma bond moves through every stage in order, but the architecture is consistent:
The Stages of Traumatic Bonding
- Love bombing: Intense idealization, excessive affection, rapid boundary-testing disguised as devotion. This phase creates the "high" the victim will spend the rest of the relationship chasing.
- Trust and dependency: The abuser becomes the primary source of validation, connection, and identity. Isolation from other support systems accelerates this.
- Criticism and devaluation: The shift begins — gaslighting, contempt, blame-shifting. The victim questions their own perceptions.
- Resignation and loss of self: The victim's identity, boundaries, and autonomous decision-making erode. They organize their life around managing the abuser's emotions.
- Addictive attachment: The cycling between cruelty and kindness becomes the organizing rhythm of the relationship. Leaving feels impossible — not because of external barriers, but because the neurochemical withdrawal is overwhelming.
If this progression sounds familiar, you may also recognize patterns described in living with and leaving a narcissistic partner — the dynamics overlap significantly because both involve systematic exploitation of attachment.
How Do I Know If What I'm Experiencing Is Actually Trauma Bonding?
Ask yourself these questions honestly:
- Does this person use unpredictable patterns of reward and punishment to keep you off-balance?
- Do you question your own perception of reality because they consistently deny or distort what happened?
- Have you become isolated from friends and family — either through direct prohibition or because maintaining those relationships creates so much conflict it isn't worth it?
- Have you lost touch with your own needs, feelings, and sense of identity?
- Is there a power differential where you feel genuinely fearful of their reaction?
- Do you simultaneously believe "this person hurts me" and "this person loves me" — and find yourself minimizing the abuse to resolve that dissonance?
If you answered yes to most of these, what you are experiencing has specific clinical characteristics and requires safety-focused intervention. The patterns described here aren't just "relationship problems" — they are markers of systematic psychological manipulation that tends to escalate.
If It's Not Trauma Bonding, What Might It Actually Be?
If you're struggling to leave a relationship but the pattern doesn't match what's described above, you're not making it up. Your pain is real. It just has a different name — and that name points to different (and more effective) help:
Attachment anxiety from early relationships can make separation feel intolerable even when the other person isn't abusing you. If your nervous system learned in childhood that disconnection equals danger, leaving any relationship — even one that isn't working — will activate survival-level distress. This is real neurobiology, just different neurobiology than trauma bonding. Understanding your attachment style can clarify what's driving the difficulty.
Grief and loss about a relationship ending, even when ending it is the right choice. You can love someone and simultaneously recognize that staying together doesn't work. That's not a bond forged through abuse — it's the ordinary, devastating cost of losing something that mattered.
Boundary wounds rooted in childhood experiences where your needs weren't prioritized. You learned to override your own compass, tolerate what shouldn't be tolerated, and call it love. That pattern requires healing — but through a lens of self-reclamation, not abuse recovery.
Codependency can make you more vulnerable to trauma bonding, but it isn't the same thing. Codependent patterns involve organizing your identity around another person's needs — which is painful and limiting, but doesn't require the intermittent abuse and power differential that define a trauma bond.
All of these deserve compassionate therapeutic attention. None of them are trauma bonding. And calling them that won't help you heal — it will point you toward frameworks designed for a different wound.
What Should I Do If I Recognize Myself in the Trauma Bonding Pattern?
If the descriptions above match your experience, your first priority is safety — not relationship repair. This is not a "both sides need to communicate better" situation. This is a situation where one person has systematically exploited the other's attachment system, and the most dangerous moment is often the point of leaving.
Research consistently shows that the period during and immediately after separation is the highest-risk window for serious violence in abusive relationships. The UK Femicide Census found that 41% of women killed by a partner or former partner had recently separated or taken steps to leave. Safety planning is not optional — it is the intervention.
Reach out to the National Domestic Violence Hotline at 1-800-799-7233 or text START to 88788. You can also visit thehotline.org or domesticshelters.org to find local safety resources. These services are free, confidential, and staffed by advocates trained specifically in domestic violence safety planning.
You need professionals who understand coercive control, not just "couples counseling." A therapist trained in trauma recovery and domestic violence dynamics can help you build a safety plan, understand the neurobiological forces keeping you attached, and begin the process of reclaiming your own perceptions and autonomy.
How Is Trauma Bonding Treated in Therapy?
Recovery from a trauma bond happens in stages — and trying to skip stages is one of the most common reasons people return to abusive relationships. The work begins with stabilization: building safety, restoring basic nervous system regulation, and reconnecting with people and resources outside the bond. This is not the time for deep processing. It's the time for ground beneath your feet.
Once safety is established, therapeutic approaches that address the body's role in maintaining the bond become essential. EMDR therapy is particularly effective for trauma bonding because it targets the way traumatic memories are stored in the nervous system — not just the narrative of what happened, but the felt sense of danger and attachment that keeps the bond alive even after physical separation. When talk therapy alone isn't resolving the pull back toward the abuser, it's often because the bond lives in the body, not in the story. If you've hit that wall, understanding why talk therapy plateaus with trauma can help clarify your next step.
Attachment-focused therapy helps rebuild the capacity for healthy connection that the trauma bond distorted — learning to distinguish between intensity and intimacy, between fear-based bonding and secure attachment. Somatic processing addresses the body patterns that maintain hypervigilance and the freeze/fawn responses that made leaving feel impossible.
The later stages of recovery involve identity restoration — the slow, powerful work of finding who you actually are underneath the adaptations the bond required. In Soul Unity Therapy, this integration is where the deepest transformation happens: reconnecting with the parts of yourself that were surrendered to survive the relationship, and discovering that those parts were never destroyed — only waiting.
Janice LaFountaine, LMFT, specializes in complex trauma recovery, coercive control, and the aftermath of trauma bonding. She serves clients throughout Washington and Idaho via telehealth and in-person sessions from her Spokane-area home office. Whether you need help understanding what you experienced or support rebuilding after leaving, therapy can help you reclaim your sense of self and reality.
Disclaimer: This content is for educational purposes only and does not constitute medical advice or establish a therapeutic relationship. If you are in immediate danger, call 911. If you need support with domestic violence, contact the National Domestic Violence Hotline at 1-800-799-7233 or text START to 88788. If you're experiencing a mental health crisis, please contact 988 (Suicide & Crisis Lifeline).
Continue reading in the Coercive Control recovery series
- The Invisible Prison: Understanding Coercive Control — the parent framework — trauma bonding almost always exists inside a larger pattern.
- Why "Narcissist" Became the Label We Can't Stop Using — the clinical precision behind naming abusive dynamics accurately.
- Living With—and Leaving—a Narcissistic Partner — the idealization-devaluation cycle that strengthens trauma bonds.
- The Financial Coercion Blueprint — how economic dependency compounds the neurobiological bond.
- Understanding Your Attachment Style — why some nervous systems are more vulnerable to intermittent reinforcement.